A Week In The Life” is a weekly Zikoko series that explores the working-class struggles of Nigerians. It captures the very spirit of what it means to hustle in Nigeria and puts you in the shoes of the subject for a week.
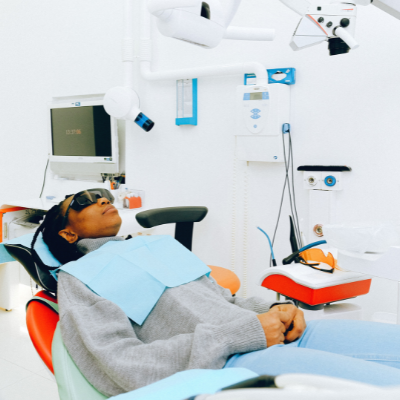
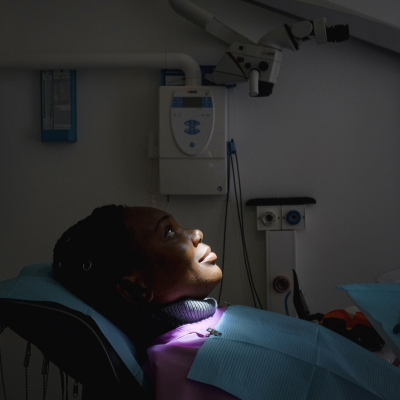
The subject of today’s “A Week In The Life” is a community health worker. Community health workers are trained to assist the healthcare team with tasks like vaccination and all-around preventive care. Our subject talks to us about some of the challenges of the vaccination program, why vaccines can’t be sold, and how to report the side effects of the vaccine.
MONDAY:
I wake up to the sound of my alarm telling me it’s time for the fajr prayer. It’s quarter to 6 a.m., and I drag myself, slowly, out of bed to say my prayer. I’m done after 30 minutes, and my clock reads 6:15 a.m. This means I have another 45 minutes to relax my eyes.
I’m up by 7 a.m., and now my day begins — I have my bath, brush my teeth and iron. I dislike ironing. It’s such a boring task. However, every morning, I’m plagued with the burden of ironing my shirts. Thankfully, my trousers don’t need ironing. After I’m done, I polish my shoes next.
After that, breakfast. I warm up leftover food from the previous day and manage to eat very little.
Then I dress up and check the mirror. “Not looking bad,” I say to myself as I dash out of the house.
The first thing the security man says to me when I get to the hospital is “Oga, you no wear nose mask today?”
On one hand, I can’t believe I forgot something so important. On the other hand, it’s understandable because fatigue has set in from wearing masks all the time. I make a mental note to get a mask when I settle in at work.
At 9:00 a.m. the vaccination exercise for the day kicks off. The crowd controller and person in charge of orientation address the crowd on what to expect from the exercise. After they’re done, we start attending to patients. Patients fall under two main groups — people who registered online and have a vaccination I.D. And patients who haven’t registered before and have to be manually registered.
My process typically goes: see if the patient has registered online. If yes, verify their details and proceed to administer the vaccine. If not, register them manually [this takes time], verify information and administer the vaccine. After injecting them, I counsel the patients on expected side effects and monitor them for about 10 – 15 minutes. While monitoring the patient, I also look at my adverse effects kit — which contains stimulants and steroids — in case of any untoward reaction.
I rinse and repeat this process until 4 p.m. when we’re done administering vaccines for the day.
At the end of each vaccination day, we hold accountability meetings where we reconcile the number of patients seen with the vials of vaccines used. We also take feedback and observations from the regulatory bodies on how to improve the whole process for the next day.
These meetings take nothing less than three hours to conclude.
Monday meetings are longer than usual, so I’m preparing my mind. I know that no matter what happens, I’ll leave the hospital by 7:30 p.m. I can’t wait to get home, complete my solats and jump into my favourite place in the world — my bed.
TUESDAY:
I have some “free” time during lunch break at work, so I spend today reminiscing about all the drama surrounding the vaccination exercise.
On the first day of the exercise, we prepared to receive 600 people in my LGA, and only 70 – 100 people showed up. This was hilarious because, in anticipation of a large crowd, the hospital brought in armed police escorts to prevent vaccine theft and to ensure the safety of health workers.
There was also the challenge of misinformation among health workers. It was difficult convincing some of my colleagues who had undergone the vaccination training to take the vaccines. After all we were taught, some of them simply did not trust the safety of the vaccine.
Lastly, there were people who wanted the vaccination card and not the vaccine itself. Their reason was that since the cards were computerised and had barcodes, it was for international purposes and this could help them get travel visas easily. This was funny to hear.
Lunch break is over by the time I snap out of my daydreams. When I get back to my duty post, there are patients waiting for me. The first patient is uncooperative and starts to shake before even seeing the injection. I spend a few minutes reassuring them that it’s a relatively painless process, but they don’t believe me. From their behaviour, I can tell that we’re going to be here for a very long time.
WEDNESDAY:
Today, I’m tired. I’m tired of one person vaccinating as many as fifty people because of the shortage of manpower. I’m fagged out by the long ass review meetings at the end of each day. More importantly, I’m stressed from constantly explaining to people that the main aim of the vaccine is to reduce the mortality rate from the Covid-19 virus and that until the second dose is administered, they should continue safety precautions like hand washing and wearing of nose masks.
I’m also tired of working long hours every day. I just want to be soft in peace.
But even in the tiredness, we move. That’s why I drag myself to have my bath and prepare for work.
At work, the NAFDAC team in charge of monitoring reactions to the vaccine is around. They’re educating people on the types — serious and non-serious — of reactions common with the vaccine. The non-serious drug reaction includes chills, mild fever, headache, pain at the injection site and weakness. The serious drug reaction reactions include anaphylactic shock, fainting, seizures, arm paralysis.
The NAFDAC team also spends some time educating people on steps to take to report any adverse reaction. This information has gingered some of my colleagues who have been sceptical about the vaccine. On our healthcare worker’s WhatsApp group, we all make plans to get our vaccines tomorrow.
THURSDAY:
I’m lowkey scared of needles but the question is, who isn’t? I’m excited to get vaccinated today, and I’ve prepared myself on what to expect.
9:30 a.m.: Took the vaccine. I kept on asking about the potency of the vaccine which made my colleagues laugh. In their words, “You’ve never worried about potency since you’ve been administering it on others, so why are you asking now?” We all laughed.
2:00 p.m.: Experienced chills and took two tablets of paracetamol to counter it. It’s not me that side effects will kill.
4:00 p.m.: Reported the chills side effects to the pharmacovigilance team of NAFDAC to help them in data collation.
7:30 p.m: Got home, prayed my solats, and did a video call with my girlfriend, the love of my life.
11:00 p.m.: Slept off in order to be properly recharged for another day on the capitalist treadmill.
FRIDAY:
I’ll be the first person to admit that the vaccination process is not perfect. There are holdups and limitations that slow down the process — system downtime, website crashes, etc. However, one thing I can vouch for is the vaccines are stored in a way that they can’t be resold by health workers.
The value chain of a vaccine is that it comes from the Oshodi central cold store to the local government’s cold store. Before vaccines leave the LGA’s cold store, it passes through a cold chain officer who distributes a realistic amount of vaccines sufficient for a team. At the end of the vaccination exercise, the empty vaccine vials are returned to this officer alongside the name and number of patients seen. After that, the cards bearing the patients names are collected and the barcodes are scanned to confirm the existence of these patients. Additionally, the number of syringes used and disposed of will be tallied against the number of vials used and patients administered.
Also, every LGA team has three supervisors who constantly monitor the vaccination activities for discrepancies. Because of how tightly controlled the process is, the highest that can happen is people paying others to help them jump a queue.
I start my day by giving a version of this speech to someone accusing health workers of selling vaccines to patients. After I’m done with my long explanation, I have a slight headache and I go to lie down.
I’m thinking about a future when I’ll move from the stress of fieldwork to a management role. I’m also thinking that the weekend is here, so I can finally rest. My plan this weekend is simple: sleep all through and be free from the world and all its stressors.
Check back every Tuesday by 9 am for more “A Week In The Life ” goodness, and if you would like to be featured or you know anyone who fits the profile, fill this form.
[donation]